Subtotal $0.00
The Key to a Pain-Free Knee After TKR
Total knee replacement (TKR) is one of the most successful procedures in orthopaedic surgery. However, a significant number of patients continue to experience anterior knee pain even after otherwise well-performed surgery. In many cases, the source of this pain is the patellofemoral joint — especially when the native patella is left unresurfaced.
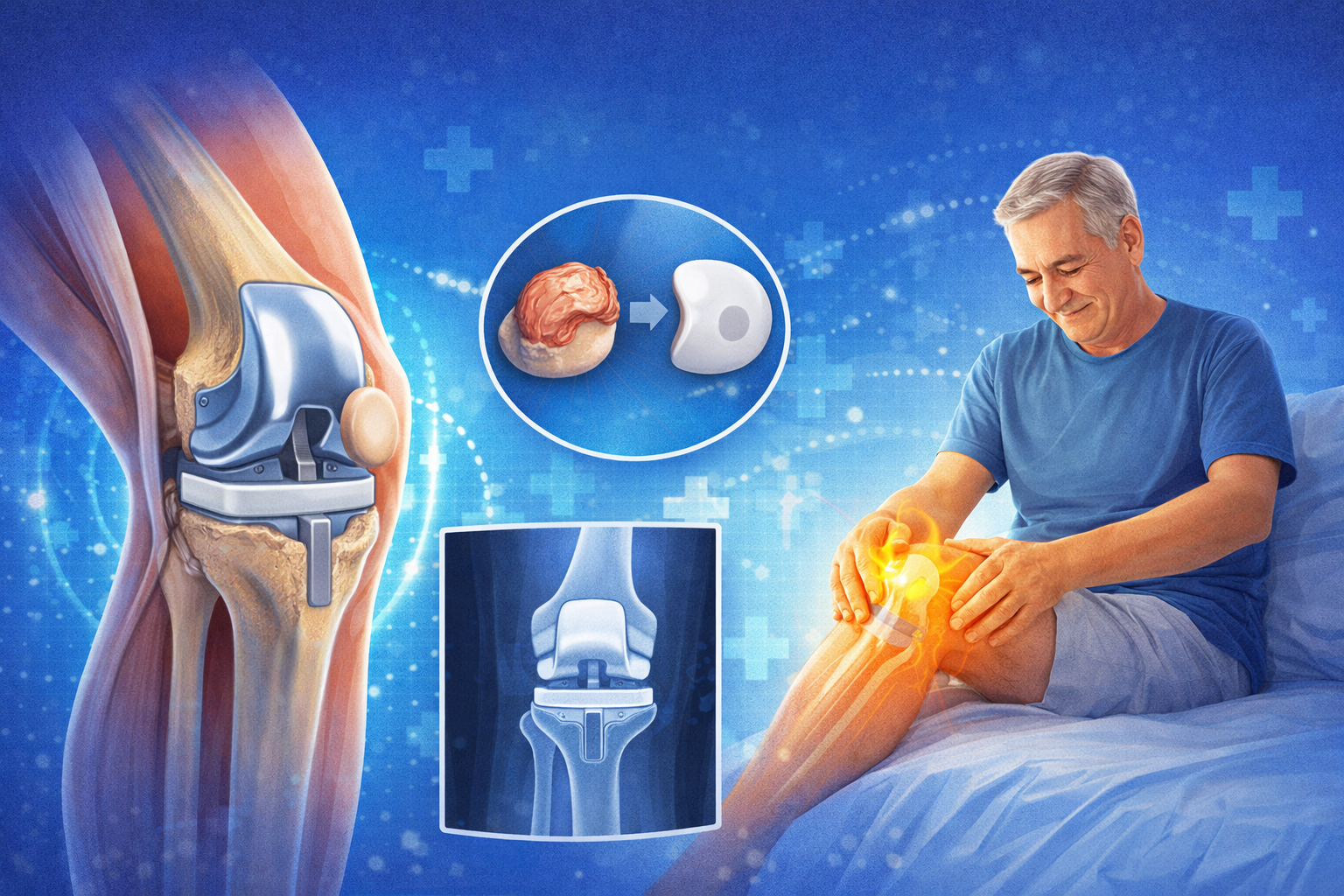
Patella replacement, or patellar resurfacing, involves replacing the diseased articular surface of the patella with a polyethylene button during TKR. While this remains a debated topic, growing evidence suggests that patellar resurfacing plays a major role in reducing anterior knee pain, improving patient satisfaction, and lowering the need for revision surgery.
Why the Patella Matters in TKR
The patella is not just a small bone in front of the knee. It is an important part of knee mechanics and contributes significantly to normal movement.
It helps by:
Increasing the efficiency of the quadriceps mechanism
Distributing force across the femoral trochlea
Protecting the front of the knee joint
During activities such as stair climbing, rising from a chair, kneeling, and squatting, the patellofemoral joint is exposed to very high forces. If the native patellar cartilage is arthritic and not replaced during TKR, these forces continue to act on a painful surface.
The Problem With Leaving the Patella Unreplaced
When the native patella is not resurfaced, it continues to articulate against the new femoral component. This can lead to:
Persistent anterior knee pain
Pain while climbing stairs or standing up from a chair
Grinding or crepitus during movement
Patellar maltracking
Patellar clunk syndrome
Need for secondary patellar resurfacing later
One of the biggest concerns is that secondary resurfacing, done after the primary TKR, often gives less satisfactory results than resurfacing performed during the original operation.
Why Patellar Resurfacing Helps
Patellar resurfacing addresses the arthritic patellofemoral surface at the time of TKR itself. By replacing the damaged cartilage surface with a properly positioned polyethylene component, the surgeon can improve patellar tracking and reduce the pain generated at the front of the knee.
The key benefits include:
Reduced anterior knee pain
Better stair-climbing comfort
Improved overall patient satisfaction
Lower rate of revision surgery
Lower chance of patellar clunk and maltracking
This is why many surgeons now consider resurfacing the patella as an important part of complete knee reconstruction.
What the Evidence Suggests
Over the years, multiple randomised trials, registry studies, and meta-analyses have evaluated patellar resurfacing versus non-resurfacing.
The overall findings consistently show that resurfaced knees tend to have:
Less anterior knee pain
Better satisfaction scores
Lower reoperation rates
Better function during activities that stress the patellofemoral joint
The rate of secondary resurfacing after primary TKR without patella replacement remains significant, and the outcomes of delayed resurfacing are usually not as good as primary resurfacing.
Technical Precision Is Essential
Patellar resurfacing can provide excellent outcomes, but only when done correctly. Surgical technique matters greatly.
Important technical principles include:
Restoring native patellar thickness
Performing a parallel and balanced patellar cut
Positioning the component correctly
Preserving patellar blood supply
Confirming central patellar tracking intra-operatively
Avoiding overstuffing of the patellofemoral joint
Poorly performed resurfacing can lead to fracture, maltracking, loosening, or excessive contact pressure. So while resurfacing has clear benefits, precision is essential.
Are There Exceptions?
Yes. Patellar resurfacing may not be ideal in every patient. Selective decision-making may be required in cases such as:
Very thin patella
Poor bone stock
Previous patellar surgery
Compromised blood supply
Rare cases where the patellar cartilage is genuinely normal
However, these are exceptions rather than the rule. In most patients undergoing TKR for advanced arthritis, the patellofemoral joint is already involved.
Why This Matters to Patients
From the patient’s perspective, the success of TKR is not judged only by the X-ray. It is judged by whether pain is relieved and daily activities become easier.
Patients commonly want to be able to:
Climb stairs comfortably
Rise from a chair without pain
Kneel or squat when needed
Return to daily, social, or religious activities
These functions depend heavily on the patellofemoral joint. If the patella remains painful, the patient may still feel dissatisfied even if the rest of the knee replacement appears well aligned.
Conclusion
Patellar resurfacing in total knee replacement is not a minor add-on — it is often the key to a more complete and pain-free result. The patella is an active participant in knee function, and untreated patellofemoral disease remains one of the commonest reasons for persistent anterior knee pain after TKR.
Current evidence strongly supports patellar resurfacing as a way to reduce anterior knee pain, improve satisfaction, and reduce the need for later revision surgery. While individual decision-making remains important, resurfacing should be strongly considered as the default approach in most total knee replacements.
A pain-free knee after TKR depends on treating the whole joint — and that includes the patella.