Subtotal $0.00
Arthroscopic ACL Mucoid Debridement with Bone Decompression for Better Long-Term Results
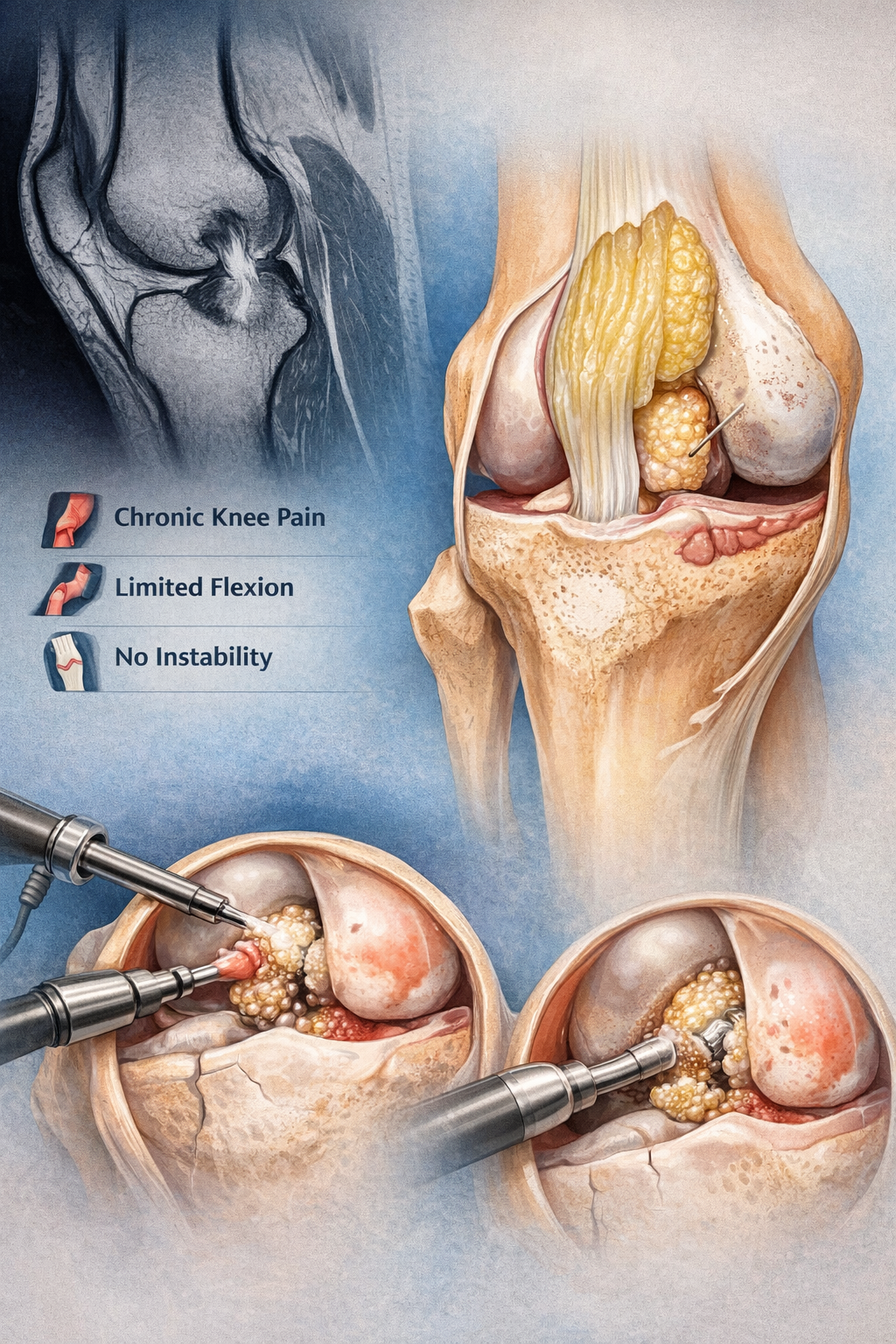
ACL mucoid degeneration (ACL-MD) is a distinct, non-traumatic condition in which the normal fibres of the anterior cruciate ligament are progressively replaced by mucoid material. Although it is increasingly recognised on MRI, it remains underdiagnosed and often misunderstood. Many patients experience chronic knee pain, restricted flexion, and functional limitation for years before receiving the correct diagnosis.
The treatment dilemma in ACL mucoid degeneration lies in choosing the right approach. Options include conservative treatment, partial debridement, complete ACL resection, and arthroscopic mucoid debridement with notch and bone decompression. Current evidence suggests that arthroscopic debridement with bone decompression offers the best long-term clinical outcome by relieving symptoms while preserving ligament function.
What Is ACL Mucoid Degeneration?
ACL mucoid degeneration is a non-inflammatory, non-traumatic degenerative process in which the normal collagen fibres of the ACL are replaced by mucoid material. Unlike an ACL tear, the ligament remains continuous, but it becomes enlarged, stiffer, and less compliant.
As the ligament thickens, it can impinge within the intercondylar notch during terminal flexion, leading to posterior knee pain and restriction of movement. In some cases, the mucoid material may extend into the adjacent bone at the tibial or femoral attachment, forming intraosseous cysts that further contribute to pain.
Clinical Presentation
Patients with ACL mucoid degeneration are usually adults between 30 and 60 years of age and often do not report a major traumatic event. The common symptoms include:
-
Chronic posterior knee pain
-
Restricted terminal flexion
-
Pain during squatting, kneeling, or stair climbing
-
Morning stiffness or activity-related swelling
-
Absence of instability
A key feature is that the knee usually remains mechanically stable. This helps distinguish ACL mucoid degeneration from a traumatic ACL tear.
MRI Findings
MRI is the diagnostic cornerstone in ACL mucoid degeneration. The most characteristic finding is the celery stalk sign, seen as linear increased signal within the ACL while preserving overall fibre continuity.
Other MRI findings may include:
-
Enlarged ACL
-
Preserved ligament continuity
-
Bone cysts at the ACL footprint
-
No marrow oedema pattern typical of acute ACL injury
MRI not only confirms the diagnosis but also helps guide treatment planning, especially when bone cysts are present.
The Treatment Dilemma
Conservative Management
Initial treatment usually includes medicines, physiotherapy, and activity modification. This may provide temporary symptomatic relief, particularly in early cases.
However, conservative treatment does not correct the structural problem. The enlarged ligament continues to impinge during knee flexion, and symptoms often persist. Long-term success rates are limited in symptomatic patients.
Arthroscopic Partial Debridement
Partial debridement removes the diseased mucoid tissue while preserving healthy ACL fibres. This can improve pain and restore flexion.
Its limitation is that it may not address the osseous component of the disease. In patients with tibial or femoral bone cysts, soft tissue debridement alone may lead to persistent or recurrent symptoms.
Complete ACL Resection or Reconstruction
Complete ACL resection is generally considered too aggressive because it may create long-term instability in a knee that was previously stable. ACL reconstruction is also not ideal in most cases, as these patients usually do not have true instability and may not require full ligament reconstruction.
The Preferred Treatment
Arthroscopic ACL mucoid debridement with notch decompression and bone cyst decompression addresses both major components of the disease:
-
The bulky mucoid ACL tissue causing impingement
-
The osseous pressure component caused by intraosseous cysts
This approach allows removal of the pathological tissue while preserving functional ACL fibres. When bone cysts are present, decompression helps eliminate an important pain source and improves the chances of long-term relief.
Why Bone Decompression Matters
Bone cysts are not incidental findings. They are part of the disease process and can generate pain through increased intraosseous pressure and periosteal stretch. Studies have shown that patients who undergo debridement combined with bone decompression generally have better outcomes than those treated with soft tissue debridement alone.
This combined procedure has been associated with:
-
Better pain relief
-
Improved knee flexion
-
Higher patient satisfaction
-
Lower re-operation rates
-
More durable long-term results
Clinical Outcome
Published studies suggest that arthroscopic mucoid debridement with bone decompression provides good-to-excellent outcomes in a high percentage of patients, with improved pain scores, better range of motion, and sustained functional recovery over time.
The success of treatment depends on proper diagnosis, detailed MRI evaluation, careful surgical planning, and a structured post-operative rehabilitation programme.
Conclusion
ACL mucoid degeneration is a distinct and progressive condition that should not be mistaken for a routine ACL tear. It commonly causes chronic knee pain and restricted flexion without instability, making diagnosis challenging.
When conservative treatment fails, arthroscopic ACL mucoid debridement with notch and bone decompression offers the most balanced and effective treatment. By addressing both the soft tissue and osseous components of the disease, this approach provides better long-term relief, preserves ligament function, and helps patients return to daily activities with improved comfort and mobility.