Subtotal $0.00
A Surgery Better Avoided
Axillary nerve neuropraxia after upper limb electrocution injury is a recognised but often under-appreciated condition. In many cases, the temptation to operate arises from uncertainty, patient anxiety, and fear of missing a structural lesion. However, in the majority of patients, surgery is best avoided.
This condition usually recovers well with conservative management. Understanding its natural history, the timing of investigations, and the risks of premature surgical exploration is essential for proper treatment.
What Happens in Axillary Nerve Neuropraxia?
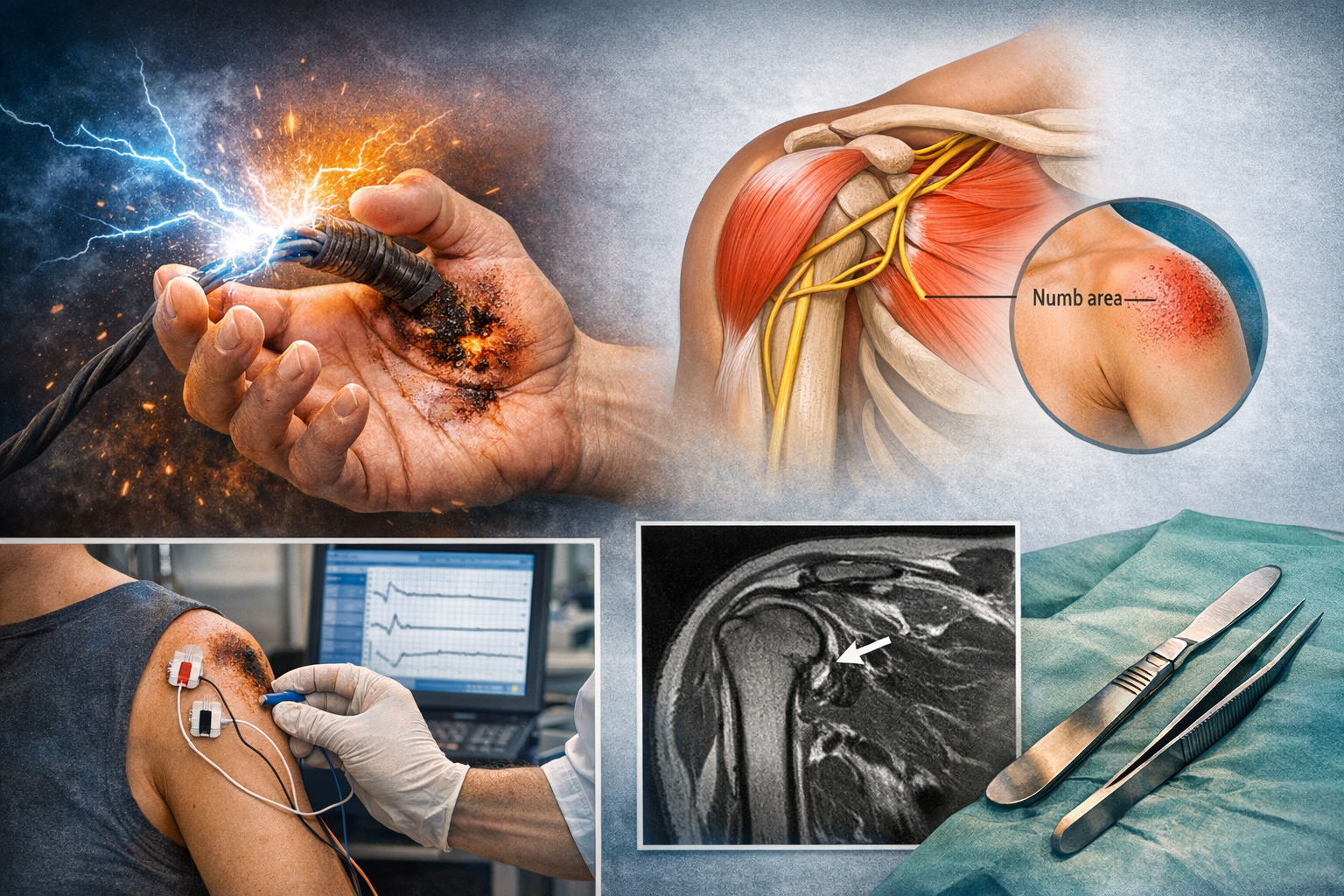
The axillary nerve supplies the deltoid muscle and a small area of sensation over the outer shoulder. After electrocution injury, this nerve may suffer a temporary conduction block, known as neuropraxia. In this type of injury, the nerve remains structurally continuous and has a strong potential for spontaneous recovery.
Electrical injuries often affect the myelin sheath without completely disrupting the nerve. This is why neuropraxia is more common than more severe injuries such as axonotmesis or neurotmesis.
Common Clinical Presentation
Patients usually present with:
-
Weakness of shoulder abduction due to deltoid weakness
-
Mild weakness in external rotation
-
Numbness or altered sensation over the lateral deltoid region
-
No major structural shoulder injury such as fracture or dislocation
A key point is the absence of associated shoulder pathology. This helps distinguish the condition from other causes of axillary nerve dysfunction.
Investigation and Its Pitfalls
Electrodiagnostic studies such as NCS and EMG are useful, but timing is very important. In the first two to three weeks after injury, these tests may be misleading. The most reliable time for testing is around three to four weeks post-injury.
MRI neurography or ultrasound may help assess nerve continuity and exclude compressive lesions such as haematoma. Plain X-rays are useful to rule out fracture or dislocation but usually do not change management.
Why Surgery Should Usually Be Avoided
1. Most Cases Recover Naturally
The majority of axillary nerve neuropraxia cases after electrocution recover fully or near-fully within three to six months with conservative care.
2. Early Surgery Carries Real Risk
Surgical exploration of the axillary nerve is not a minor procedure. It carries risks of:
-
General anaesthesia
-
Injury to surrounding blood vessels and structures
-
Iatrogenic damage to the nerve
-
Scar formation that may interfere with recovery
-
Longer rehabilitation and unnecessary psychological stress
3. Early Diagnostic Uncertainty Does Not Justify Exploration
If the injury is neuropraxia, surgery offers no benefit. If a more severe injury exists, waiting for a short observation period usually does not worsen the final outcome.
4. Intraoperative Findings Often Do Not Change Management
In many explored cases, the nerve appears continuous or only mildly swollen. These findings rarely justify major intervention and often confirm that surgery was unnecessary.
When Surgery May Be Considered
Surgery should be reserved for selected patients with clear indications, such as:
-
No clinical or electrophysiological recovery by 3–4 months
-
Imaging showing nerve discontinuity or a compressive lesion
-
Progressive neurological deterioration
-
High-voltage injury with extensive local tissue destruction
-
Associated vascular injury requiring surgery nearby
These are exceptions, not the rule.
Conservative Management Protocol
Acute Phase (0–4 Weeks)
-
Pain relief and anti-inflammatory treatment
-
Sling only for comfort, avoiding prolonged immobilisation
-
Gentle physiotherapy to maintain range of motion
-
Baseline electrodiagnostic testing planned for 3–4 weeks
-
Clear patient reassurance about the likely favourable recovery
Subacute Phase (4–12 Weeks)
-
Repeat clinical evaluation at regular intervals
-
Electrodiagnostic follow-up as needed
-
Progressive physiotherapy with active-assisted exercises
-
Monitoring of sensory and motor recovery milestones
Decision Phase (12–16 Weeks)
By this stage, recovery is usually evident in most patients. If deltoid function remains absent and investigations show no reinnervation, then surgical consultation becomes reasonable.
Clinical Message
The most important decision in axillary nerve neuropraxia after electrocution is often the decision not to operate. Confident diagnosis, correct timing of investigations, and patient counselling are central to successful management.
Most patients improve with time, physiotherapy, and observation. Premature surgery may add risk without improving outcome.
Conclusion
Axillary nerve neuropraxia following upper limb electrocution injury is a condition with an excellent natural history in most cases. Conservative management should be the first-line approach, with surgery reserved only for a small and carefully selected group of patients.
Proper timing of EMG and nerve conduction studies, careful clinical follow-up, and specialist input where required can prevent unnecessary surgery and support optimal recovery.